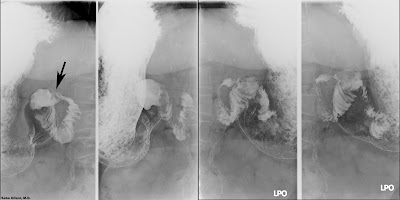
The CECT images above are from a patient who underwent sleeve gastrectomy (blue arrow) and experienced worsening abdominal pain in the weeks that followed. She was admitted with sepsis. There are necrotic areas within the spleen and multiple rim enhancing collections of air and fluid (red arrows) compatible with abscesses. Left upper quadrant fluid collections (sterile and infected) are a known complication of bariatric surgery.
REFERENCES
Blachar A and Federle MP. Gastrointestinal complications of Roux-en-Y gastric bypass surgery in patients who are morbidly obese: findings on radiography and CT. AJR Am J Roentgenol 2002;179:1437-42.
Yu J, Turner MA, Cho SR, et al. Normal anatomy and complications after gastric bypass surgery: helical CT findings. Radiology 2004;231:753-60.