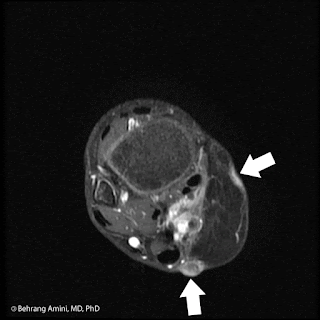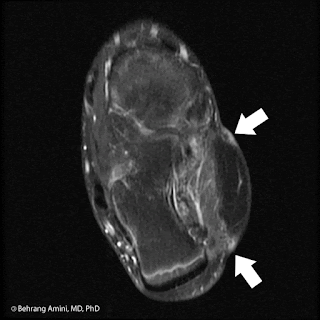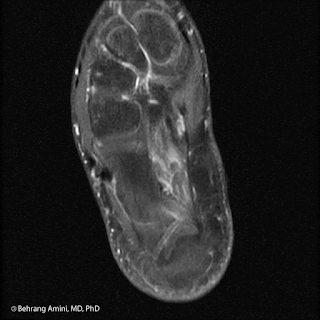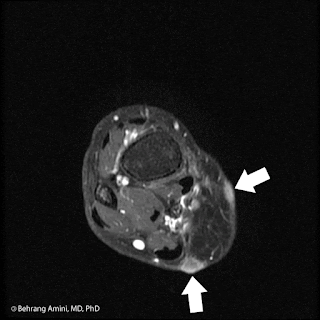
Patient with history of radiation therapy for head and neck cancer. Radiation field extended into the supraclavicular nodal stations. CT shows an osteoid producing soft tissue mass to the right of midline. Bone scan and PET show uptake in the lesion, as well as contralateral lymph nodes. PET shows an FDG-avid lung nodule. T1-WI post-contrast MRI with FS shows a peripherally enhancing soft tissue mass.
The incidence of radiation-associated sarcomas of bone and soft tissue is about 0.1%. They are more commonly seen in patients with breast cancer, lymphoma, head and neck malignancies, and gynecologic cancers. The distribution of primary cancers is likely related to the larger numbers of patients with these cancers and the high survival rates for these tumors.
The majority of radiation-associated tumors are soft tissue sarcomas, with bone sarcomas making up about 20-30% of cases. The majority are high grade and aggressive. The most common soft tissue sarcomas are unclassified pleomorphic sarcoma (UPS, formerly MFH), followed by angiosarcoma (particularly in breast cancer), fibrosarcoma and leiomyosarcoma (particularly in retinoblastoma). The most common bone sarcomas are osteosarcomas.
The latency between radiation and sarcoma ranges from as little as a few months to 54 years. The average is 7 to 16 years. In breast cancer, the average is 10 to 11 years (4-8 years for angiosarcomas). In childhood cancers, the average latency is between 12 to 13 years.
Risk factors include, dose (Rarely seen with low doses: <40 Gy), age at exposure, concomittant chemo exposure (particularly alkylating agents) and genetic tendency (e.g., Li-Fraumeni syndrome).